Ariel Sánchez
It consists of the hypofunction of the parathyroid glands, with a decrease in the level of circulating hormone and hypocalcemia.
Pathophysiology
It is a rare disease. Its most frequent cause is the removal or irreparable damage of the parathyroid tissue in the course of thyroidectomies or other cervical surgical interventions. It can occur spontaneously in two ways: the first, idiopathic hypoparathyroidism, in which the parathyroid glands are atrophied or absent. The second, pseudohypoparathyroidism, in which the glands are hyperplastic and overactive, although the hormone they secrete is ineffective and cannot keep calcium at its normal level.
The mechanism of glandular damage in postsurgical hypoparathyroidism is not entirely clear, although it is suggested that it is the result of ischemia; it reflects the magnitude of the dissection and hemostasis required, and therefore its incidence is higher after oncological neck surgeries than after partial thyroidectomies for benign goiter. There is no relationship between the occurrence of tetany and the presence or absence of parathyroid tissue in the surgical specimen. Other rare causes of hypoparathyroidism due to glandular damage are 131I irradiation, hemochromatosis, and infiltration of the glands by metastatic malignant tissues.
All other cases of hormonal-deprived hypoparathyroidism fall into the category of "idiopathic." There are neonatal instances, due to agenesis or hypoplasia of the glands. A form of glandular hypofunction attributable to autoantibodies, or to parenchymal replacement by fatty tissue and fibrosis, can occur sporadically or in families. A genetic disorder is known, transmitted in an autosomal recessive manner, capable of causing hypofunction of several endocrine glands, including the parathyroid glands; Generally, autoantibodies directed against various organs (thyroid, adrenal, ovaries, etc.), and recurrent mucocutaneous candidiasis are found. While the majority of idiopathic hypoparathyroidism was believed to be due to autoimmunity, It is currently accepted that the main cause is a defect in the calcium receptor or sensor (CaR), located in the membrane of parathyroid cells; Due to specific mutations, an intrinsic activation of the same occurs, which always interprets extracellular calcium levels as “high” - even if they are low - and sends signals that inhibit the secretion and release of PTH.
Pseudohypoparathyroidism is a rare inherited disorder associated with distinctive skeletal defects (Albright's osteodystrophy): short stature, short neck, brachydactyly generally affecting the fourth and fifth metacarpals and metatarsals, curved radius, and various exostoses. The facies is rounded. This disease is due to the lack of response of the constituent organs to PTH. Due to this refractoriness of the peripheral tissues, there is a hypersecretion of the hormone. The basis of the abnormality is not in the secretion of an abnormal PTH, but in the defective transmission of the hormonal message through the receptor and the adenyl cyclase system in the membranes of the target cells. In affected subjects, the stimulatory subunit of protein G (Gs) is missing,
The hypocalcemia of hypoparathyroidism is caused by a decrease in the passage of calcium from the bone to the blood, by a lower intestinal absorption of calcium, and by a reduction in its tubular resorption. The activity of renal 1-alpha-hydroxylase falls, with lower synthesis of calcitriol and low serum levels of this metabolite. The other important consequence of the lack of PTH is the elevation of serum phosphorus, due to an increase in the renal threshold for phosphate.
Symptoms and signs
Most of the manifestations are due to increased irritability of the nervous system, both central and peripheral.
The typical attack of tetany begins with paresthesias in the hands and around the mouth, which can lead to a sensation of numbness in these areas and spread to the extremities and the entire face. The muscles begin to stiffen and eventually contract, this spasm being more frequent in the hand and forearm than in the foot and leg. The first change is adduction of the thumb, followed by flexion of the metacarpophalangeal joints and extension of the interphalangeal joints, without separation of the fingers (midwifery hand, Fig. 76-1) and finally flexion of the wrist and elbow. The pain is variable, and can be severe. There is a very understandable subjective reaction to this alarming condition, with tachycardia and hyperpnea, and occasionally paleness and sweating.
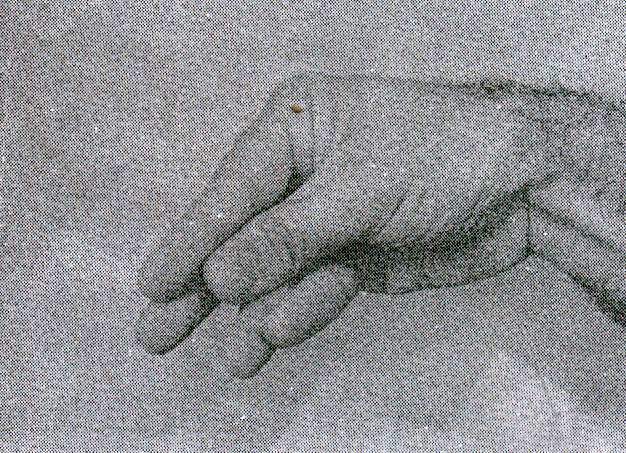 Trosseau sign |
Minor degrees of neuromuscular hyperexcitability may not manifest spontaneously, and it is necessary to provoke the typical signs (latent tetany). The Chvostek sign consists of percussion of the facial nerve just below the zygomatic arch and about 2 cm anterior to the earlobe with the finger; the response can range from a slight contraction of the angle of the mouth (which is frequent and unspecific) to the contracture of all facial muscles on the side under investigation. The more specific Trousseau sign is sought by inflating the handle of a sphygmomanometer placed on the arm above the systolic pressure. It is considered positive if a typical carpal spasm is obtained within 2 minutes. This takes about 5-10 seconds to give way once the cuff is deflated; if it disappears immediately,
Other manifestations may be some difficulty in speech, and even frank laryngeal spasm; dysphagia or intestinal cramps; dyspnea and bronchospasm. Tremors, myoclonus, and seizures may occur in children. Table 77-1 summarizes the clinical features of neuromuscular irritability caused by hypocalcemia.
|
Table 76-1. Clinical features of neuromuscular irritability caused by hypocalcemia
|
In cases of chronic hypocalcemia, several organic disorders can be seen: small and irregular calcifications, visible on lateral radiographic films of the skull, and corresponding to the basal ganglia of the brain; papilledema; dry and flaky skin; brittle nails and rough, brittle hair; waterfalls; heart failure, etcetera. Alterations in the electroencephalogram are common in these cases.
Study methodology
Positive diagnosis requires recognizing the manifestations of true tetany in the patient's symptoms and documentation of hypocalcemia. It should be remembered that there are tetanias in the presence of normocalcemia, attributable to hyper or hypokalaemia, or hypomagnesemia, or respiratory alkalosis. The latter is the most frequent cause; A decrease in calcium occurs, partly because alkalosis increases the calcium-binding capacity of plasma proteins, and partly because organic acids accumulate in circulation and combine with the ion. Furthermore, alkalosis per se increases neural excitability.
Hypocalcemia and hyperphosphatemia (although this does not appear constantly and its magnitude is variable) will lead to suspicion of hypoparathyroidism, which must be certified by means of a PTH dosage: if the value found is undetectable or very low, there will be no diagnostic doubts. If there is normal serum PTH, but at that time the calcaemia is not markedly decreased, hypocalcemia can be induced by infusion of EDTA in order to demonstrate subnormal secretion of the hormone. If the PTH level is elevated concomitantly with frank hypocalcemia, the likely diagnosis will be pseudohypoparathyroidism.
Calciuria is generally low; serum alkaline phosphatase is usually normal.
The differential diagnosis makes it necessary to rule out hypoproteinemia (serum calcium drops 0.064 mg / dl for every gram of decrease in albuminemia below its normal range), which is present in malnourished patients or those with chronic liver failure, chronic kidney failure, hypovitaminosis D
Calcemia should be requested in: 1) cases with manifest tetany, or in patients with latent tetany, which is only evidenced by the semiological maneuvers already described; 2) children with convulsive pictures, 3) adults with unclear neurological pictures, and 4) the postoperative period of cervicotomies.